Climate change is likely to impact human health in a number of ways. On the one hand, we might expect decreased mortality from extreme cold, but the flip-side is a dramatic increase in warm extremes and heat waves. The young and the elderly, as well as the poor—who are less likely to have access to modern air conditioning, etc., are most at risk. The toll of the unprecedented heat wave in Europe of summer 2003, where more than 30,000 lives were lost, is a possible harbinger of the impact of future, more frequent and intense heatwaves, and to a lesser extent, so are the European heat waves of 2006 and 2010 and, in North America, of 2006 and 2010.
Other weather extremes may have human health impacts. In some cases, such as the physical damage and loss of life from land falling hurricanes, this is obvious. But there are many other examples. Intense rainfall events leading to flooding can cause physical harm or create conditions that favor the spread of disease or lead to various ailments. Drought conditions pose the obvious threat of limiting fresh water supply, but they can also favor disease and malnutrition. Once again, the impacts fall disproportionately on the poor, who are the least able to afford clean water, electricity, and modern health care.
| Predicted Climate Change | Anticipated Effect on Human Health |
|---|---|
| On land, fewer cold days and nights | Reduced mortality from cold exposure (virtually certain) |
| More frequent heat waves | Increased mortality from heat, especially among the young, elderly, and those in remote regions (virtually certain) |
| More frequent floods | Increased deaths, injuries, and skin and respiratory disease incidence (very likely) |
| More frequent droughts | Food and water shortages; increased incidence of food- and water-borne disease and malnutrition (likely) |
| More frequent strong tropical cyclones | Increased mortality and injury, risk of flood- and water-borne disease, and incidence of post-traumatic stress disorder (likely) |
| More extreme high-sea-level events | Increased death and injury during floods; health repercussions of inland migration (likely) |
(Note: Predicted climate change listed in order of decreasing certainty)
© 2015 Pearson Education, Inc.

Climate change is also likely to lead to the spread of various types of infectious disease. Many of these diseases are spread by so-called vectors—pests, such as insects and rodents, which are capable of spreading the disease far and wide. In many cases, the ranges of vectors are restricted by climate. Diseases such as West Nile Fever and Malaria, for example, are spread by mosquitoes. Temperate regions with killing frosts are thus relatively inhospitable to the disease, as they interrupt the life cycle of the vector and thus the disease itself. As the globe warms and cold regions retreat poleward, we can expect the regions where diseases currently classified as "tropical diseases" are endemic to spread well into the extratropics. The outbreak of West Nile Virus in New York State in 2005, for example, was likely due to an unusually warm winter, which allowed mosquitoes to persist through much of the year.
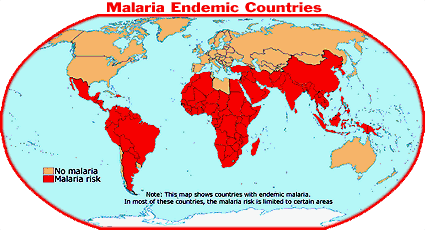
The story is not quite as simple as that, however. Consider malaria. There are reasons why malaria can be found far into the subtropics of Asia and South America, but not, in the U.S. This has to do with the fact that industrial nations, like the U.S., have adequate resources to eradicate Malaria through the use of appropriate health practices and technology that is not available to third world nations.
Moreover, the connection with climate is a bit more complex than warmer temperature = more malaria. Here at Penn State, we have experts who are studying the potential impacts of warming temperatures on the spread of malaria. The problem is complicated, in part, because it is not just the average temperature that determines how rapidly the malaria parasite can reproduce. It turns out that there is a threshold dependence on temperature (recall our discussion of thresholds in the context of climate tipping points). The malaria parasite reproduces at an exponentially greater rate above a particular threshold temperature, roughly 20°C. This is why highland tropical African cities such as Nairobi, with an elevation of nearly 5000 feet and a mean annual temperature of 19°C, are generally free of malaria, even while surrounding lowland regions must contend with the disease. This threshold dependence on temperature also implies that one must not only consider the mean temperatures, but also the variability of temperatures, to assess possible impacts on the spread of malaria. Let us demonstrate this through an example.
Think About It!
Consider two hypothetical cities. City A has an annual mean temperature of 18°C and a standard deviation of 1°C. City B has an annual mean temperature of 17°C and a standard deviation of 3°C.
Which city is more likely to see an increase in spread of malaria if both warm by 1°C on average?
City A
City B
If you answered "City B" you are correct!
Even though it will remain 1°C colder than City A, it will spend considerably more time above the critical temperature of 20°C, because of its greater temperature variability.
The threshold dependence of malaria on temperature means that the problem of projecting climate change influences on malaria is even more challenging than we might have thought. One must be able to project not only how mean temperatures will change, but also how the diurnal temperature range, the seasonal cycle, and even the inter-annual variability might change. And since there is much uncertainty about whether, e.g., ENSO events will be larger or smaller as a result of anthropogenic warming, there is much uncertainty, too, in how the amplitude of inter-annual variability in temperatures will change in many parts of the world.
Of course, temperature is not the only climate variable that might influence malaria. Rainfall matters too: the fewer breeding spots available for the disease vector (anopholes mosquitoes), the less likely that malaria takes hold. Unfortunately, as we have seen, projections of future changes in precipitation in regions such as Kenya is quite uncertain (see the Precipitation and Drought page of Lesson 7), largely because of uncertainties in ENSO. This makes projecting impacts of climate change on infectious disease particularly challenging.
